DebtDynamics – North America | Battered and bruised: a guide to distress in healthcare
[Editor’s note: The first paragraph has been amended post publication to correctly state certain figures to match the chart below.]
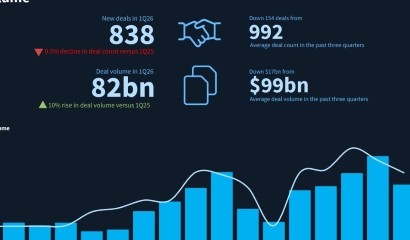
The US healthcare sector has been beset by malaise in recent months, with the number of restructuring cases lurching to 49 in 2023 from 23 the previous year. Prospects show little sign of improving in 2024, with a dozen Chapter 11 cases already on the table since 1 January, representing USD 3bn of liabilities. Overall, in the year to date (YTD) to 20 March, there have been 35 Chapter 11 applications for total debt of USD 6.5bn, with 12 of these coming from healthcare companies, or 34% of all Chapter 11 filings, per Debtwire’s Restructuring Database.
Approximately one-third of all firms that filed for Chapter 11 protection between January 2022 and March 2024 have been healthcare focused, leading to questions about why there has been such an outbreak of distress in the sector.
Healthcare companies currently battle a variety of headwinds. Chief among these are reimbursement challenges stemming from Medicare cuts, changes in revenue cycles under the No Surprises Act, high labour expenses fuelled by soaring inflation, and steeper funding costs.
Cuts to reimbursement rates for physician pay have depleted medical services providers’ collectibles since July 2022. Medicare first cut its rate by 2% in 2022, and then further reduced the repayment rate by 3.37% in January 2024.
The No Surprises Act – a federal law passed by the government to protect patients covered under individual or group health plans from unexpected hospital bills – came into effect on 1 January 2022. The act forbids health providers from charging patients directly for the portion of medical bills that exceed insurance protection for certain emergency services. It also established an independent dispute-resolution process between plans and providers. Multiple dispute-resolution cases have accumulated since the legislation was introduced, creating a significant collectibles backlog for hospitals.
In addition, some companies tried to take advantage of lower borrowing rates during the coronavirus (COVID-19) pandemic, fuelling growth through debt-backed acquisitions. Surging interest rates put a strain on these over-levered firms, which was further exacerbated by faltering cash flows created by the legislative measures implemented by the government.
Debt-funded growth operations backfire
The two largest healthcare companies by liability to file for Chapter 11 in 1Q24 YTD are Invitae Corporation and Cano Health, with combined debt of USD 2.4bn out of the total of USD 3bn of healthcare liabilities in distress during the period.
Invitae, a medical genetics company, went through a liability-management exercise in February 2023 in an attempt to revive its loss-making fortunes. As part of its corporate restructuring, Invitae divested several business entities and privately exchanged USD 306m 2% senior convertible notes due 2024 for USD 275m 4.5% series A convertible senior secured notes due 2028 and a cash component. The group had embarked on a purchasing spree between 2019 and 2021, acquiring a string of business entities that manifest in a negative bottom-line in subsequent years. Invitae continued to burn cash throughout 2023 and, despite workforce reductions and other cost-saving initiatives, as well as the divestment of its Citizen and Natera divisions in the second half of the year, the company filed for Chapter 11 on 14 February, with USD 1.5bn of liabilities outstanding.
Cano Health, a Florida-based primary care provider, is another example of a healthcare company failing after pursuing an aggressive acquisition strategy funded by debt between 2018 and 2022. The company launched its liability-management exercise in 2023, setting out a plan to optimize operations by exiting certain markets and consolidating some others, but eventually had to file for Chapter 11 in February, with USD 900m of debt. Cano’s management had been relying on third-party medical cost reductions and the optimization of its core Medicare Advantage and ACO REACH assets; however, reimbursement rate cuts by Medicare further drained the company of liquidity.
In need of medical attention
We expect to see more companies struggle as the year rolls on. As at 20 March, there were another 13 healthcare companies rated as distressed based on their Likely-To-Distress (LTD) scores powered by Debtwire’s NextGen data, and some 28 more in the stressed universe. Below is the list of companies in Debtwire’s distressed universe:
Source: Debtwire
Of the four companies on the list with liabilities over USD 2bn, Global Medical Response (GMR) is the largest, with debts totaling USD 5.3bn. The air and ground ambulance company engaged with advisors and creditors in 2023 to amend and extend its USD 3.7bn term loan and USD 600m senior notes maturing in 2025. GMR’s operations deteriorated in late 2022-early 2023 following two fatal air accidents and persistent inflationary pressure on wages, leaving the company trying to balance retaining human capital and high financial leverage.
Team Health Holdings, a physician-staffing provider, completed a liability-management exercise in February for its remaining term loan B, senior secured PIK loan and revolving credit facility. However, the company still needs to address its USD 714m notes due February 2025, while its cash-generating capacity is constrained and leverage remains high. Team Health’s operations are likely to be further impacted by lower collectibles stemming from the Medicare rate cuts and extended dispute resolutions determined by the No Surprises Act.
Dialysis provider US Renal Care completed a distressed debt exchange in summer 2023 in order to optimize its capital structure, but its debt load of USD 2.4bn appears unsustainable given decreased cash flows.
EyeCare Partners also faces challenges servicing its debt because of a very limited capacity to generate cash. The company cites staffing shortages and higher inflationary costs as the main reasons for poor cash generation, which are the same underlying problems afflicting US Renal Care.
We anticipate the healthcare restructuring pipeline getting even busier as the year progresses, with many services providers beleaguered with third-party payment overheads stemming from Medicare’s revised payment rates, the backlog of medical bills stuck in dispute-resolution processes and high inflationary labour costs. While the rate of inflation increase has slowed based on the latest Consumer Price Index data from the US government, we believe there needs to be a significant fall before healthcare companies are able to climb off their sickbeds and start to recover their liquidity and leverage.